Polycystic Ovary Syndrome (PCOS) is a hormonal disorder in women of reproductive age. According to the CDC, it affects nearly 5 million, which accounts for roughly 6 – 12% of women and girls of reproductive age in the US. Women with PCOS have higher than normal levels of androgen (a male hormone) in the body, which impacts their monthly ovulation process. It means the ovaries do not regularly release/develop eggs. Some of the eggs may develop into cysts (little sacs filled with liquid-follicles), build up in the ovaries, and get enlarged in size.
PCOS is a group of symptoms affecting women’s ovaries and their normal ovulation process. It is characterized by three main features: cysts in the ovaries, irregular periods (disrupted ovulation process), and excessive male hormones called androgens, whose signs include hirsutism, acne, and hair loss). According to the NHS, if a woman is having at least 2 out of these three conditions, their doctor may diagnose them with PCOS and suggest them for further physical examination and medical/lab testing for the same.
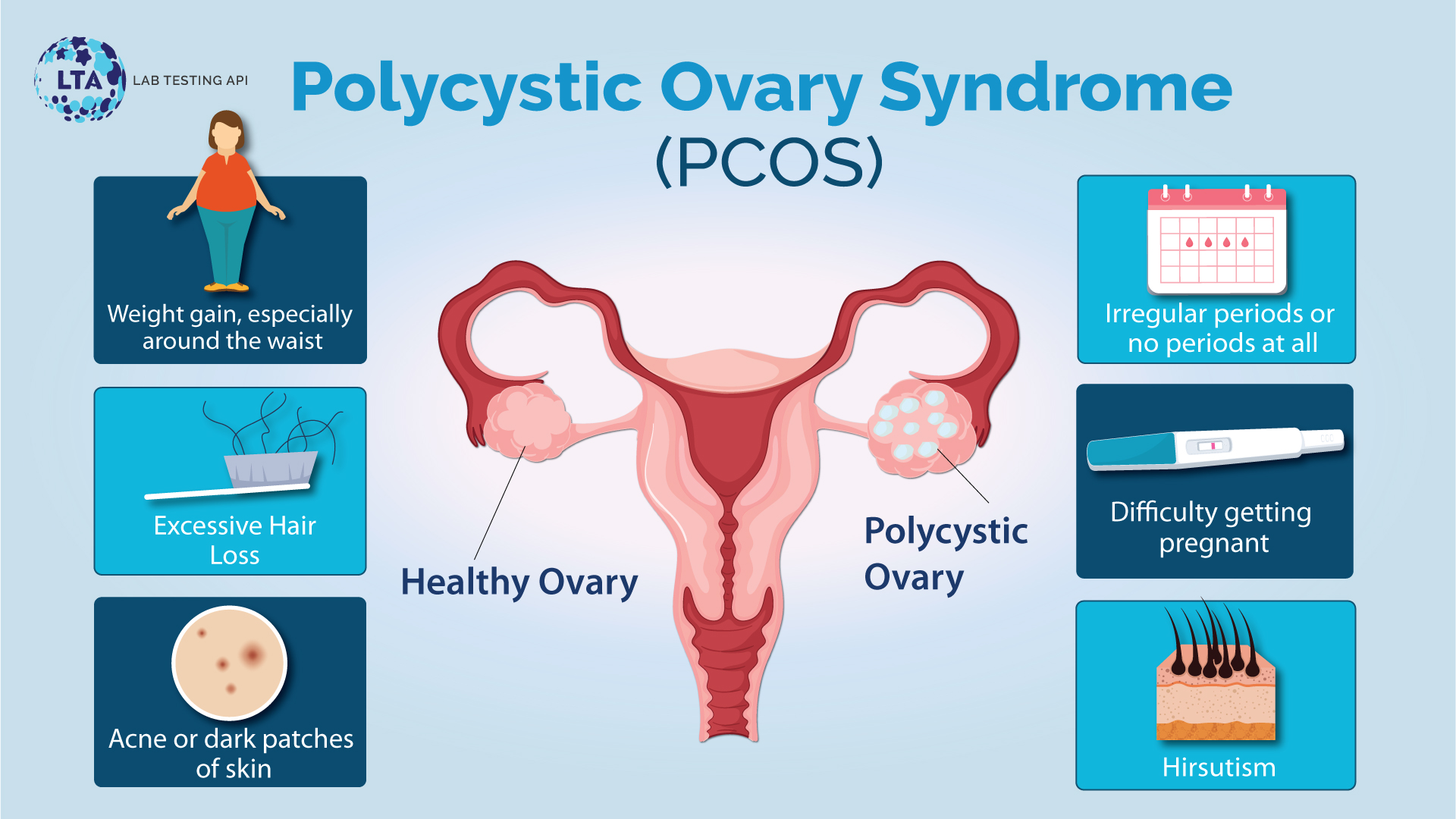
The classical signs and symptoms of PCOS include:
PCOS is also associated with an increased risk of developing Type 2 Diabetes. The CDC, in its research “PCOS (Polycystic Ovary Syndrome) and Diabetes”, states that women with PCOS are often insulin resistant which means their bodies are making insulin but not using it effectively. On one hand, this situation increases the risk for Type 2 Diabetes. On the other hand, it may cause the ovaries to work differently by producing higher than usual levels of androgens, which in turn cause many of the signs and symptoms of PCOS.
The exact cause of PCOS is still a mystery among doctors, but heredities play an important role, and evaluating one’s family history may assist in understanding its cause. PCOS is generally related to increased levels of two hormones in the body: insulin and androgens. Being overweight or obese can also increase insulin levels and make PCOS symptoms worse.
Your health care provider will ask about your medical history and your symptoms. As discussed above, if your doctor found at least 2 of the three main characterizing features of PCOS, he/she will diagnose you with PCOS and ask for a physical exam and medical lab testing. You may be asked for:
An Ultrasound. This test is used to evaluate the size of the ovaries and to check if there are cysts. It can also be used to check the endometrium, the thickness of the lining of the uterus.
Blood tests. The blood tests may look for high levels of androgens and other hormones. The other biomarkers like blood glucose, cholesterol, and triglyceride may also be checked.
Lab Testing API offers a range of blood tests to determine your risk of having the polycystic ovarian syndrome, a common hormonal disorder in women. PCOS Blood Test is a comprehensive test that measures follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels, as well as sex hormone-binding globulin (SHBG) – all of which exert their effects on the gonads. It also measures testosterone, a hormone responsible for the development of male sexual characteristics. An individual can order their blood work at discounted rates through our website, and all lab orders include a physician’s order.
Many factors play a role in the effective treatment of PCOS. They may include your age, the severity of your symptoms, your overall health, and your future planning to become pregnant (1).
If you are planning to become pregnant, your doctor may suggest you to:
On the other hand, if you are not planning to become pregnant, your doctor may advise you to do the above, as well as:
To maintain good health, it is recommended to make positive lifestyle changes to prevent as well as treat hormonal disorders and conditions. The best treatment for PCOS includes timely diagnosis and the further appropriate steps that can help overcome the syndrome and make the journey towards conception a success (2).
Our next blog will discuss some myths associated with PCOS.
Written by Dr. Shikha Sharma, Reviewed by Dr. Harshi Dhingra
